A new AMYPAD paper entitled “Quantification of amyloid PET for future clinical use: a state-of-the-art review” has been published in the European Journal of Nuclear Medicine and Molecular Imaging.
In this state-of-the-art review, methods for quantification of static amyloid PET scans are summarised and compared along with a discussion of the overall utility of amyloid PET quantification in routine clinical practice, observational research, and clinical trials.
Abstract:
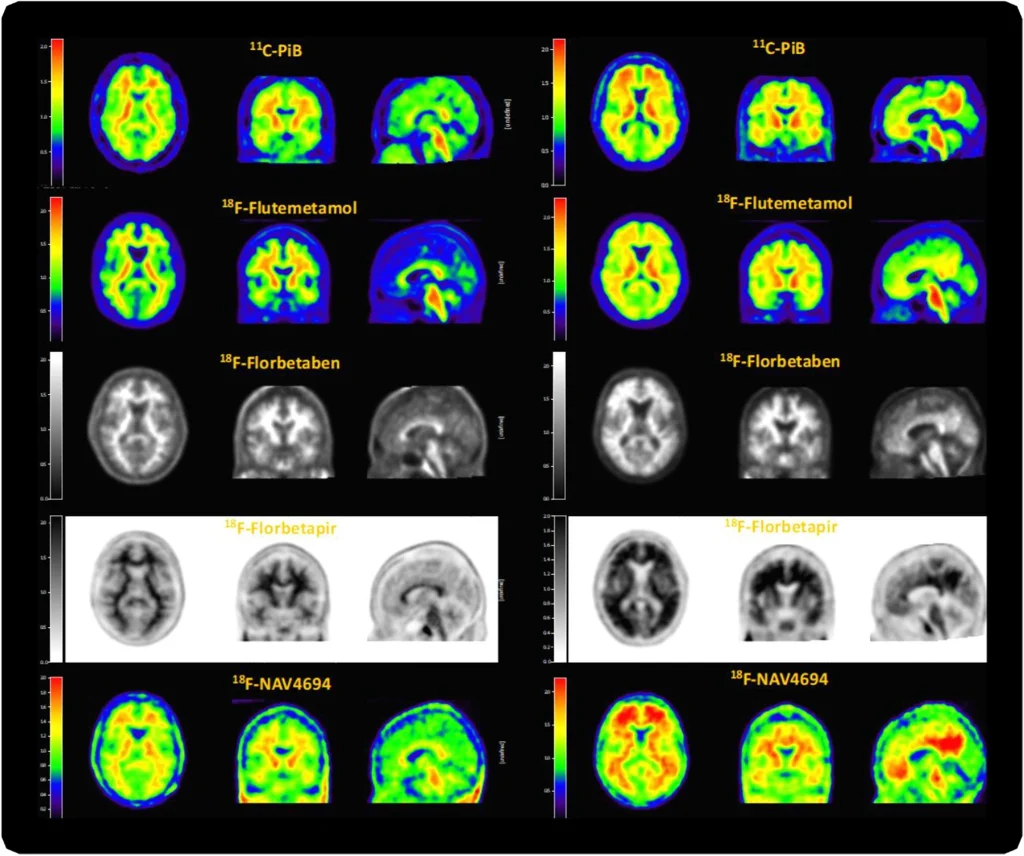
Amyloid-β (Aβ) pathology is one of the earliest detectable brain changes in Alzheimer’s disease (AD) pathogenesis. The overall load and spatial distribution of brain Aβ can be determined in vivo using positron emission tomography (PET), for which three fluorine-18 labelled radiotracers have been approved for clinical use. In clinical practice, trained readers will categorise scans as either Aβ positive or negative, based on visual inspection. Diagnostic decisions are often based on these reads and patient selection for clinical trials is increasingly guided by amyloid status. However, tracer deposition in the grey matter as a function of amyloid load is an inherently continuous process, which is not sufficiently appreciated through binary cut-offs alone. State-of-the-art methods for amyloid PET quantification can generate tracer-independent measures of Aβ burden. Recent research has shown the ability of these quantitative measures to highlight pathological changes at the earliest stages of the AD continuum and generate more sensitive thresholds, as well as improving diagnostic confidence around established binary cut-offs. With the recent FDA approval of aducanumab and more candidate drugs on the horizon, early identification of amyloid burden using quantitative measures is critical for enrolling appropriate subjects to help establish the optimal window for therapeutic intervention and secondary prevention. In addition, quantitative amyloid measurements are used for treatment response monitoring in clinical trials. In clinical settings, large multi-centre studies have shown that amyloid PET results change both diagnosis and patient management and that quantification can accurately predict rates of cognitive decline. Whether these changes in management reflect an improvement in clinical outcomes is yet to be determined and further validation work is required to establish the utility of quantification for supporting treatment endpoint decisions. In this state-of-the-art review, several tools and measures available for amyloid PET quantification are summarised and discussed. Use of these methods is growing both clinically and in the research domain. Concurrently, there is a duty of care to the wider dementia community to increase visibility and understanding of these methods.
Congratulations to the authors: Hugh G. Pemberton, Lyduine E. Collij, Fiona Heeman, Ariane Bollack, Mahnaz Shekari, Gemma Salvadó, Isadora Lopes Alves, David Vallez Garcia, Mark Battle, Christopher Buckley, Andrew W. Stephens, Santiago Bullich, Valentina Garibotto, Frederik Barkhof, Juan Domingo Gispert and Gill Farrar.
You can read the paper here.